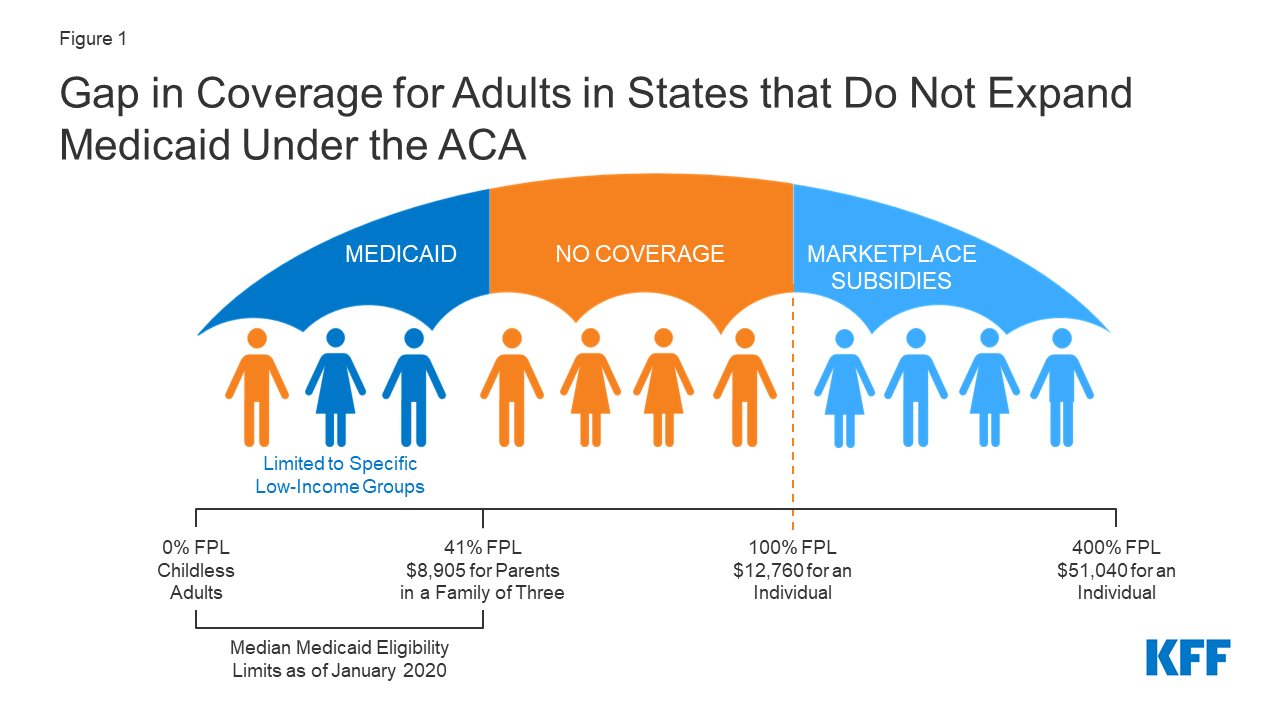
The Coverage Gap
What if you make too much to be eligible for Medicaid but not enough to afford adequate health insurance?
One of the most immediate after-effects of the pandemic were the millions of Americans that have lost health insurance due to layoffs and lost employment. Though millions have received coverage through qualifying for Medicaid over the past year, 12 states have not expanded Medicaid, which has led more than 2 million Americans to fall into the “coverage gap” - where adults make more than their state’s eligibility for Medicaid but below poverty, the minimum income eligibility for insurance subsidies through the Affordable Care Act marketplace.
For historical context, the coverage gap is largely due to the Supreme Court decision of National Federation of Independent Businesses v. Sebelius (NFIB), which transformed the initial intention of the ACA from making Medicaid expansion a requirement for all states to an option. In the aftermath, we saw states implement Medicaid largely along party lines, leaving most folks caught in the coverage gap left in the South. However, federal incentives to cover the startup costs for expansion and research showing how Medicaid expansion ultimately help states save costs over time (primarily via mental health, corrections, and uncompensated care)
At a time when many are losing critical health coverage during a health crisis, these eligibility gaps leave many without an affordable coverage option. What’s most frustrating for me is that the majority of families that fall into this gap are employed in very low-wage jobs, employed part-time, or with a fragile or unpredictable connection to the workforce. They’re gig workers, day laborers, restaurant workers - arguably among the hardest-working folks in our nation.
There are a few potentially promising policy tailwinds that I’ll summarize below with the incoming Biden administration, but there doesn’t seem like to be a straightforward solution here. There are still plenty of ways to more meaningfully improve access to care for those caught in the coverage gap in the short-term.
Policy Insights: Public Option
Biden proposed a public option through the ACA insurance marketplace that would allow individuals caught in the coverage gap to receive coverage free of premiums and cost-sharing. This change would not require state funding or approval in the 12 states that have yet to expand Medicaid eligibility. However, this proposal wasn’t included in the COVID-19 relief bill, and it remains an open question on how to support individuals caught in the coverage gap, especially without the Democratic votes needed to pass as legislation.
The tricky part is getting coverage to poor people in the Medicaid coverage gap without creating incentives for states that have already expanded Medicaid to drop the expansion
Biden’s nomination for the head of the CMS Chiquita Brooks-LaSure seems aligned in prioritizing Medicaid access; however her federal agency would have to work with states at an arm’s length via Medicaid waivers, alternative payment models, and via other incentives given the state-oriented nature of Medicaid administration and expansion.
Idea: Redesigning Health Benefits for the Uninsured
There have been a number of startups like Mira and Sidecar Health who are able to provide much more affordable health coverage at 40-80% below commercial rates by prioritizing virtual care or through urgent care partnerships. Though it’s not clear that this is the type of longitudinal care that these populations ultimately need, it certainly seems better than being completely uninsured. Vitable Health is one of the more interesting approaches focusing primarily on smaller employers that employ <50 folks who are not mandated to provide health insurance by the ACA but may still want to offer their employees something.
I wonder if there are other ways to reinvent health benefits for this population - working closely with larger companies (e.g., Construction Firms, Fedex, etc…) that employ a good percentage of their workers as independent contractors that don’t receive full benefits. For those that lose productivity on high contractor turnover or see costs from covering workers compensation, perhaps there is an employer incentive to subsidize cost-effective coverage that could increase contractor retention in a centralized setting (e.g., monthly offering of virtual or onsite urgent care coverage)
Another service that could benefit this population is a marketplace for these alternative self-pay options that could help contractors make an informed decision based on their family’s medical needs on remaining uninsured vs covered through one of these alternative options. Over time, a platform like this could collect enough data to drive ROI for employers who may want to subsidize these plans to drive employee usage.
Idea: Tying Medicaid Eligibility to Job Loss
Fewer than 15% of qualifying patients end up enrolling for insurance plans through the marketplace even if they qualify for what the industry calls “special enrollment periods” (SEPs) - windows of time for individuals to buy into insurance outside of the normal November-December annual open enrollment window. Unsurprisingly, the most common SEP qualification is due to loss of employment which affects 9.7M people every year and likely significantly more last year due to the pandemic. Though the Biden administration has created a special enrollment period from now until May 21, 2021, it’s no surprise why so many patients drop out of this leaky funnel for enrollment into insurance.
What if we could better tie Medicaid auto-eligibility to job loss as part of an off-boarding process in a more integrated fashion to the opt-in COBRA coverage that some folks get today? We could also automate enrollment into Medicaid through SNAP and use of other state or federally-funded services that folks access (e.g., public schools, subway subsidies)
Big thanks to Mina Iskarous, Seth Joseph, and Brian Nguyen for the comments and suggestions in pre-reading an early draft of this piece. Would love to hear from folks that work specifically with this population to better understand gaps in their care and needs beyond insurance. Am definitely still getting up to speed on the latest here, so greatly appreciate feedback and suggestions on where I can learn more.
See below for some other thoughts and ideas that didn’t make it into the post as I was digging in if interesting!
Current Medicaid Expansion Strategy
In today’s political climate, it seems unlikely that a public option would pass both the House and the Senate, so the federal strategy in incentivizing Medicaid expansion seems to be offering states really juicy financial incentives to do so likely via legislation. The below piece from TIME does a decent job highlighting the potential proposal, but wanted to highlight this sound-byte here.
Under the existing system, the federal government shares Medicaid costs with states and covers 90% of the costs for each state’s expansion group. The proposal put forth by the Energy and Commerce Committee makes that more generous: it proposes that for any state that newly expands Medicaid, the federal government would increase what it pays for all non-expansion Medicaid enrollees by 5 percentage points for two years. that extra 5% in federal funds would more than cover the states’ cost of expanding Medicaid, according to a new analysis from the Center on Budget and Policy Priorities
- TIME Democrat’s Push to Expand Medicaid
Other Ideas
Offer something similar to Aetna’s Flexible Five plan for employees that don’t have full insurance - essentially 5 free passes to the most common preventative healthcare service lines.
Still not sure why employers that have a lot of contractors would be incentivized here to subsidize something like this, but maybe the company is still profitable even in a complete FFS framework?
Virtual (and longitudinal) interdisciplinary care similar to what Amazon is doing across state lines but specifically catered to a population that has a variety of complex medical and social needs. From the brief virtual and telephone interactions I’ve had with uninsured patients working at East Harlem Health Outreach Partnership (Mt Sinai’s free clinic), there are many aspects of a high-touch and interdisciplinary model that could be productized in a virtual setting to follow patients longitudinally. More to come on this potentially in a future post…